Michelle RobertsDigital health editor

 Getty Images
Getty Images
Meningitis B (MenB) is the strain behind an outbreak of cases in Kent in which two people have died, the government’s health agency has confirmed.
An 18-year-old school pupil in Faversham, named as Juliette, and a 21-year-old student at the University of Kent were confirmed to have died from the infection.
There have been 15 cases in the area, according to the the UK Health Security Agency (UKHSA), and four of these have been confirmed in a laboratory to be MenB infections.
The agency announced it will open a targeted MenB vaccination programme at the Canterbury Campus Halls of Residence at the University of Kent in the coming days.
It added that this may be expanded as it assesses the risk to the wider population.
But the UKHSA confirmed the primary focus remains on preventative antibiotics treatment and has asked anyone who visited Club Chemistry in Canterbury on 5, 6 or 7 March to come forward for treatment as a “precautionary measure”.
More than 30,000 students, staff and families in the Canterbury area are being contacted by the UKHSA.
What are meningitis and ‘invasive’ meningitis?
Meningitis is an infection of the protective membranes that surround the brain and spinal cord.
It can affect anyone but is most common in babies, young children, teenagers and young adults. It can be very serious if not treated quickly.
The cause of the infection – either certain bacteria or viruses – can be determined by tests.
Bacterial meningitis is rarer but more serious than viral meningitis. It can lead to blood poisoning or sepsis, and can affect the brain.
This acute, severe infection is known as invasive meningitis. It means the infection has invaded into the blood stream or brain linings.
Both people who have died in the invasive meningitis outbreak in Kent are believed to be aged between 18 and 21.
MenB is the strain behind most cases of meningococcal disease in the UK.
In the most recent full year, 2024-2025, there were 378 cases of invasive meningococcal disease, according to official data.
Is there a meningitis vaccine?
Two vaccines protect against the main causes of meningitis and septicaemia.
The MenACWY vaccine offers protection against four types of bacteria that can cause meningitis – meningococcal groups A, C, W and Y – and is offered to teenagers aged 14 years old.
The MenB vaccine helps protect against meningococcal group B bacteria and is recommended for babies aged eight weeks, followed by a second dose at 12 weeks and a booster at one year.
Meningitis can sometimes occur as a complication of some other infections, meaning several other vaccinations can also help protect people.
A six-in-one vaccine given to young children – also known as the DTaP/IPV/Hib/Hep B vaccine – offers protection against diphtheria, tetanus, whooping cough, hepatitis B, polio and Haemophilus influenzae type b (Hib).
A pneumococcal vaccine offers babies protection against serious infections caused by pneumococcal bacteria, including meningitis.
The MMRV vaccine – which replaced the MMR vaccine in January 2026 – offers infants protection against measles, mumps, rubella and chickenpox.
Generally, it takes a couple of weeks to get the fullest protection from a vaccine and some require booster doses.
Why aren’t teenagers vaccinated against MenB?
The MenB vaccine was added to the UK NHS childhood immunisation programme for babies born on or after 1 July 2015.
That means current teenagers will not have been able to have it.
Young babies are vaccinated because they are more likely to get invasive infections more often than other age groups, and their bodies are less likely to be able to fight them off.
However, research suggests the MenB vaccine is not great at preventing transmission of the infection from one person to another, doesn’t target all the different B bacteria strains and doesn’t provide protection for particularly long.
UK vaccine experts have therefore concluded that it isn’t cost effective to offer the MenB vaccine to adolescents, and the NHS does not currently offer a catch-up programme.
Some parents have paid to vaccinate their teens privately. High street pharmacies offer a full course of two doses for around £220.
The vaccine does not contain any live bacteria and cannot cause meningococcal disease.
Given the severity of the situation in Kent, a small targeted vaccination programme will begin starting with students resident at Canterbury Campus Halls of Residence at the University of Kent in the coming days.
The vaccination programme may be expanded further as the UK Health Security Agency continues to asses any ongoing risk to other populations. For now, it says the priority remains for those offered antibiotics to come forward as this is highly effective at preventing the disease and transmission.
How do I find out whether I’m up to date on my vaccines?
Contact your GP to find out which vaccines you’ve already received, or look at your red book.
Vaccine coverage has fallen since the Covid pandemic, meaning fewer children and teens are protected against a range of diseases.
Anyone who missed getting the MenACWY vaccine at school can get it for free before their 25th birthday.
The MMR vaccine is free for anyone who missed getting it when they were younger, regardless of their age.
What meningitis signs should you look out for?

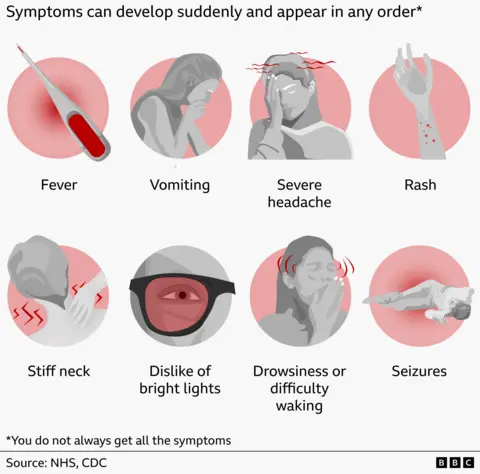
Symptoms can develop suddenly and can include:
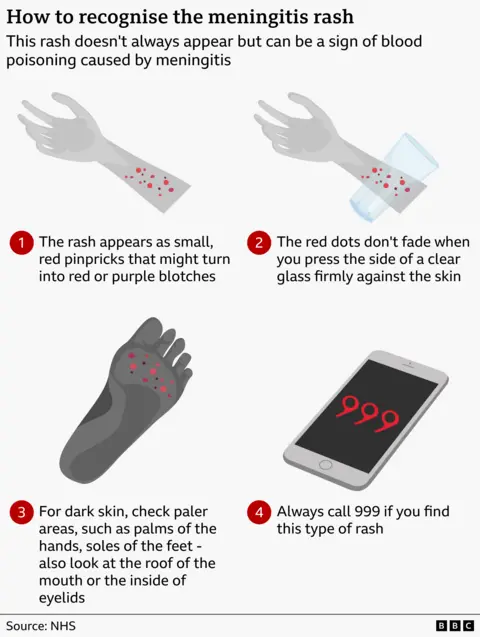
- A rash that doesn’t fade when pressed with a glass
- Sudden onset of high fever
- Severe and worsening headache
- Stiff neck
- Vomiting and diarrhoea
- Joint and muscle pain
- Dislike of bright lights
- Very cold hands and feet
- Seizures
- Confusion/delirium
- Extreme sleepiness/difficulty waking

How is meningitis spread?
Some people carry bacteria in their nose or throat without getting sick, but spread it to others in spit or saliva through coughs and sneezes, kissing and sharing utensils.
The infection can also be spread by someone with meningitis, although this is less common.
It’s possible to get meningitis more than once.
Outbreaks of meningococcal disease are rare, but can occur in settings where people group together, such as college campuses or entertainment venues.
Why is sharing vapes a risk for spreading meningitis?
Health Secretary Wes Streeting has warned that the MenB strain could be spread through sharing vapes or drinks.
“It doesn’t spread very easily,” he told the House of Commons on Tuesday.
“The bacteria is passed to others after a long period of close contact. For example, with living with someone in shared accommodation, through prolonged kissing or sharing vapes and drinks.”
Many young people carry the bacteria in their nose or throat without getting ill or developing any symptoms, but when students are mixing closely and intimately in large numbers, that increases the risk of spread.
How can you stop the spread of meningitis?
The best way to stop the disease spreading is to give antibiotics to people who may have come into contact with it.
As a precautionary measure, free antibiotics are being offered to people who visited Club Chemistry in Canterbury on March 5, 6 and 7, or are close contacts of confirmed cases.
People who live on the University of Kent campus at Canterbury are also eligible.
What to do if you think you or a friend has meningitis
Anyone becoming unwell with symptoms of meningitis and septicaemia should seek medical help urgently at the closest Accident and Emergency Department or by dialling 999.
Early treatment can be lifesaving.
Students in the affected area of Canterbury are being advised to trust their instincts – and not to wait for all symptoms to appear or for a rash to develop before seeking help via their GP or the 111 service. They are also asked to check on friends who feel unwell.
“Students are particularly at risk of missing the early warning signs of meningitis because they can be easily confused with other illnesses such as a bad cold, flu or even a hangover,” warn health officials.

